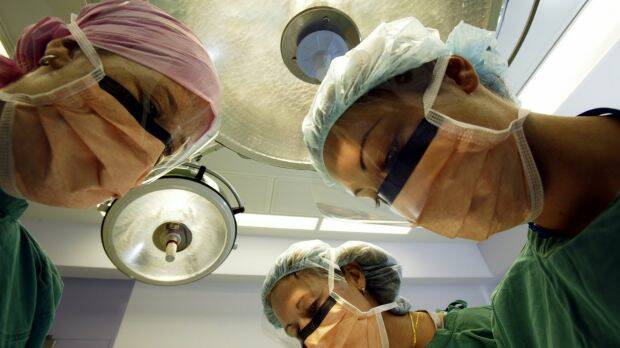
It took six years and the testimony of five surgeons, but one mother received justice on Friday when Murrumbidgee Local Health District was ordered to pay her more than $1 million in damages.
MLHD was found to have acted negligently in relation to an incisional hernia repair at Wagga Base Hospital in 2010, after which the mother of three was left suffering from a severe post-op infection.
Returning to the hospital just six days after her surgery, it was clear by July 16 2010 when the 46-year-old was admitted to a Canberra Hospital, she had developed a severe infection which required urgent surgical intervention.
Five surgeons were consulted during the Supreme Court trial proceedings, with Judge Campbell ruling the defendant had breached its duty in failing to recognise an infection.
All of the surgeons agreed that the infection suffered was a foreseeable and significant risk - especially considering the enhanced risk given the patient was a smoker, obese and had a low incision from a previous caesarean.

One of the surgeons described the case as a nightmare.
“This patient was waiting for an infection – this was on the cards right from the outset,” the surgeon said.
After the initial procedure in 2010, the woman went on to undergo another five surgeries and various treatments until September 2011, claiming ongoing pain, discomfort, scarring and psychological injury had restricted her daily life.
In determining the damages for the case, Judge Campbell said the hernia repair would have been successful, had the negligence not occurred and surgical drains been used.
“She would have gone on to lead a normal unrestricted life and would not have required the multiplicity of operations that followed,” the ruling stated.
The damages covered various past and future economic and non-economic losses, with a total figure of $1,005,509 awarded to the plaintiff.
FULL JUDGMENT
JUDGMENT
BACKGROUND
The plaintiff, Mrs Tinnock, sues the defendant, Murrumbidgee Local Health District, for personal injuries allegedly suffered by her as a result of complications of surgery provided at the Wagga Wagga Base Hospital as a public patient.
The primary surgery was the repair of an incisional hernia performed by a surgical registrar, Dr Justin Gundara, under the supervision of Dr Michael Payne, a specialist general surgeon. That surgery was undertaken on 7 June 2010. Further surgery was carried out on 15 June 2010 to drain a seroma which had developed. This second procedure involved the application of a VAC dressing. Dr Payne carried out a third procedure on 27 June 2010 to close the abdominal cavity which accommodated the VAC dressing.
There is no doubt that by 16 July 2010, when Mrs Tinnock was admitted to the Calvary Hospital in Canberra, she had developed a severe infection which required urgent surgical intervention. There is also no doubt that that severe infection was associated with the surgical mesh which had been placed over the hernia dissection to promote healing and “reinforce” the area affected by the surgery (313.5-14T). There is no question that this is a standard approach to repairing an incisional hernia.
The issues in the case relate to the cause and origin of the infection; was it avoidable; when it ought to have been evident to a specialist general surgeon; and what ought to have been done to treat it.
There is also no question that the Health District is vicariously liable for any tortious conduct of Dr Gundara or Dr Payne.
Overview of the plaintiff’s case
To make good her claim for damages, Mrs Tinnock relies upon the tort of trespass to the person, and in particular battery. Her case in this regard is that she did not consent to Dr Gundara performing the operation.
If unsuccessful in her claim for damages for battery, Mrs Tinnock advances a case in negligence. This claim is put by reference to alternatives. First, with regard to the primary surgery, it is said that an ordinary specialist general surgeon exercising and professing to have the special skill associated with that profession would have taken the precaution of inserting negative pressure surgical drains to substantially reduce or eliminate the risk of the development of post-surgical infection. In the alternative, in relation to the second and third procedure, the plaintiff says that reasonable care on the part of a surgeon required the adoption of the precautions of:
diagnosing the presence of the infection; and
either removing the mesh as the probable source of infection, or treating Mrs Tinnock as an inpatient with intravenous antibiotics for a prolonged period, say of one month.
It is said that had the surgical drains been utilised, the infection would probably have been avoided; notwithstanding the failure to take that step, the severe consequences which ensued could have been avoided by taking the alternative steps at the time of either the second or third procedure. In this regard, of course, it is said that reasonable care on the part of a surgeon of ordinary skill would have diagnosed the infection at the early stage when Mrs Tinnock re-presented at the hospital on 13 June 2010; if not, then when the VAC cavity was closed at the third procedure.
Overview of the defendant’s case
The defendant says that Mrs Tinnock’s case in battery cannot be made good because she consented to the first operation being carried out which consent extended to its performance by the surgical registrar under the supervision of Dr Payne. The defendant otherwise joins issue on the claim in negligence.
An earlier iteration of the defence pleading s 5I Civil Liability Act 2002 (NSW) (‘the Act’), that the harm suffered by Mrs Tinnock was the result of the materialisation of an inherent risk, was abandoned before trial. The defence based on s 5O of the Act was abandoned in written submissions because the expert evidence did not establish that Dr Payne’s omission to employ negative pressure drains was a particular approach that was widely accepted by peer professional opinion as competent professional practice. Rather, the evidence was that there was no established practice, or school of thought, one way or the other. The evidence demonstrated that the use of surgical drains depended upon the particular circumstances of the actual operation carried out by the surgeon and on the particular surgeon’s individual professional judgment at the time. I did not understand this evidence to indicate that surgical drains were regarded merely as ‘optional extras’ adding no therapeutic value. Rather, there were no fixed rules governing their use.
No defence of contributory negligence is said to be available.
THE PLAINTIFF’S PRIMARY CASE: TRESPASS TO THE PERSON
It seems sensible to deal with Mrs Tinnock’s claim in battery first as it turns on the single question of consent.
Legal principles
Battery is one of the three forms of trespass to the person recognised by Australian common law. The others are assault and false imprisonment. A defendant who directly causes physical contact with a plaintiff will commit a battery unless the defendant proves that the defendant was “utterly without fault”: Croucher v Cachia [2016] NSWCA 132 at [21]-[23]; (2016) Aust Torts Reports ¶82-279 at 67,633-67,634.
In X v The Sydney Children’s Hospital Network (2013) 85 NSWLR 294; [2013] NSWCA 320 at 298 [12], Basten JA said:
“The general principle of the common law is that non-consensual medical treatment involves an assault, thus constituting both a criminal offence and a tort.”
The law’s approach is underpinned by the “principle of personal inviolability”.
In Dean v Phung [2012] NSWCA 223; (2012) Aust Torts Reports ¶82-111, Basten JA (with whom Beazley JA (as her Honour then was) and Macfarlan JA (on this point) agreed) said at 66,347 [48]:
“In the therapeutic context, the defence to the tort of trespass to the person is consent. Where there has been an ostensible consent, which is later challenged, the convenient starting point is to consider the validity of the consent, rather than asking whether it has been obtained by fraud.”
While accepting that the principles informing the content of consent in criminal and civil law need not be identical, the approach of the High Court of Australia in the common law rape case of Papadimitropoulos v The Queen (1957) 98 CLR 249; [1957] HCA 74 has generally been followed. At 260-261 a unanimous Court explained:
“It must be noted that in considering whether an apparent consent is unreal it is the mistake or misapprehension that makes it so. It is not the fraud producing the mistake which is material so much as the mistake itself. But if the mistake or misapprehension is not produced by the fraud of the man, there is logically room for the possibility that he was unaware of the woman’s mistake so that a question of his mens rea may arise. …. For that reason it is easy to understand why the stress has been on the fraud. But that stress tends to distract the attention from the essential inquiry, namely, whether the consent is no consent because it is not directed to the nature and character of the act. The identity of the man and the character of the physical act that is done or proposed seem now clearly to be regarded as forming part of the nature and character of the act to which the woman’s consent is directed. That accords with the principles governing mistake vitiating apparent manifestations of will in other chapters of the law.”
The Court of Appeal for England and Wales applied the same principle in R v Richardson (Diane) [1999] QB 444. There the question was whether a dentist whose right to practice had been suspended was guilty of assault because the apparent consent of a number of patients was vitiated by mistake about her status as a dentist. The dentist had failed to disclose that her right to practice had been suspended. The prosecution argued that the operative mistake was a mistake about the identity of the person performing the act. It was argued that there was no distinction to be drawn between an unqualified person impersonating a dentist and an otherwise qualified dentist whose right to practice had been suspended. The Court said (at 450) that there was:
“… no basis for the proposition that the rules which determine the circumstances in which consent is vitiated can be different according to whether the case is one of sexual assault or one where the assault is non-sexual. The common element in both these cases is that they involve an assault, and the question is whether consent has been negatived. It is nowhere suggested that the common law draws such a distinction. The common law is not concerned with the question whether the mistaken consent has been induced by fraud on the part of the accused or has been self-induced. It is the nature of the mistake that is relevant, and not the reason why the mistake has been made. In summary, either there is consent to actions on the part of a person in the mistaken belief that he was other than he truly is, in which case it is assault or, short of this, there is no assault.
In essence, the Crown contended that the concept of the “identity of the person” should be extended to cover the qualifications or attributes of the dentist on the basis that the patients consented to treatment by a qualified dentist and not a suspended one. We must reject that submission. In all the charges brought against the defendant the complainants were fully aware of the identity of the defendant. To accede to the submission would be to strain or distort the everyday meaning of the word identity, the dictionary definition of which is “the condition of being the same””.
This approach was accepted as correct in Australian common law in Dean v Phung at 66,348-66,349 [53]-[54].
The important point for the present case is that the concept of the identity of the person does not extend to cover the qualifications or attributes of the particular professional, provided he or she is otherwise qualified.
I should say that in R v Tabassum [2000] EWCA Crim 90; [2000] 2 Cr App Rep 328, the defendant was convicted of indecent assault for touching the breasts of three women, each of whom mistakenly thought him to be medically qualified. However, the mistake was not as to identity but as to the act, the Court of Appeal for England and Wales holding that because the women consented “to touching for medical purposes not to indecent behaviour … there was consent to the nature of the act but not its quality” (337 [38]).
I have spent this time discussing these authorities because Mrs Tinnock’s case in battery is that she was mistaken as to the identity of the person who would undertake the surgery. She did not say that she was mistaken as to the nature or quality of the procedure proposed. Nor was there any mistake as to its intended therapeutic nature.
So far as the legal onus is concerned, I record that Basten JA in Dean v Phung (the other members of the Court agreeing) held that where consent validly given is in dispute, the defendant bears the burden of proof: 66, 350 [59]-[63]. Leeming JA took a different view in White v Johnston (2015) 87 NSWLR 779; [2015] NSWCA 18 at 807 [130]. Barrett JA agreed at 782 [4]. Emmett JA (at 785-6 [18]) agreed that it was for the plaintiff to prove that the treatment was “wholly non-therapeutic … if that was how an absence of valid consent were to be established”. His Honour did not expressly embrace Leeming JA’s conclusions about “the broader question of the onus of proving consent”. His Honour certainly did not demur. So far as my researches have disclosed, this difference of opinion of the Court of Appeal has not been resolved. I am prepared to assume in Mrs Tinnock’s favour that the later decision of White v Johnston does not apply for the purpose of this case. I will apply Dean v Phung. I acknowledge that the Court in White v Johnston did not purport to expressly overrule Dean v Phung in this respect and that Leeming JA’s observations on “the broader question” were obiter dictum.
Application of principles
Approaching this question I bear in mind, as Leeming JA pointed out in White v Johnston by reference to Papadimitropoulos and other authorities (at 795 [68]), the essential enquiry is about consent to the nature and quality of the act. In Papadimitropoulos in the passage quoted at [16] above the Justices said:
“The identity of the man and the character of the physical act that is done or proposed seem now clearly to be regarded as forming part of the nature and character of the act to which … consent is directed.” [my emphasis]
This gives rise to two related questions: first, in the circumstances was Mrs Tinnock mistaken inasmuch as she believed the operation would be performed by Dr Payne and no-one else; and secondly, if so, was that a mistake about the nature and character of the operation vitiating her apparent consent. After all, Dr Gundara was a legally qualified medical practitioner in the course of qualifying as a general surgeon who would be working under the direct supervision of Dr Payne. I must say I am inclined to think that even if the first question is answered favourably to Mrs Tinnock, her mistake did not go to the nature and character of the act to be performed and accordingly would not vitiate her consent to the procedure.
The law of consent as it affects the tort of battery in the context of the provision of medical treatment is accepted in Australia as having been correctly stated by Bristow J in Chatterton v Gerson [1981] QB 432; Rogers v Whittaker (1992) 175 CLR 479; [1992] HCA 58 at 490 [14]; Dean v Phung at 66, 348 [50]. Bristow J at 442-3 said:
“In my judgement what the court has to do in each case is to look at all the circumstances and say “Was there a real consent?” I think justice requires that in order to vitiate the reality of consent there must be a greater failure of communication between doctor and patient than that involved in a breach of duty if the claim is based on negligence. When the claim is based on negligence the plaintiff must prove not only the breach of duty to inform, but that had the duty not been broken she would not have chosen to have the operation. Where the claim is based on trespass to the person, once it is shown that the consent is unreal, then what the plaintiff would have decided if she had been given the information which would have prevented vitiation of the reality of her consent is irrelevant.
In my judgement, once the patient is informed in broad terms of the nature of the procedure which is intended, and gives her consent, that consent is real, and the cause of the action on which to base a claim for failure to go into risks and implications is negligence, not trespass. Of course, if information is withheld in bad faith, the consent will be vitiated by fraud.”
No allegation of fraud is made in the present case. The allegation is simply, “the plaintiff did not consent to Dr Justin Gundara carrying out the surgery” (third amended statement of claim [8D]).
By reference in part to Chatterton v Gerson, the unanimous High Court in Rogers v Whittaker (at 490) said:
“… the phrase “informed consent” is apt to mislead as it suggests a test of the validity of a patient's consent. Moreover, consent is relevant to actions framed in trespass, not in negligence. Anglo-Australian law has rightly taken the view that an allegation that the risks inherent in a medical procedure have not been disclosed to the patient can only found an action in negligence and not in trespass; the consent necessary to negative the offence of battery is satisfied by the patient being advised in broad terms of the nature of the procedure to be performed.” [footnotes omitted]
I think that a similar dichotomy informs questions about the identity of the person performing the operation so far as that may go to the nature and character of the procedure. The facts in Chappel v Hart (1988) 195 CLR 232; [1998] HCA 55 demonstrate that the identity of the surgeon in terms of his or her skill and experience can be a factor material to the patient, and relevant to the probability of the occurrence of a foreseeable risk incidental to the surgery proposed. However, the relevant breach on the part of the surgeon in that case was the failure to warn of the specific risk of a complication that materialised. The evidence showed that the skill of the surgeon was relevant to causation inasmuch as (on one view of it) the risk of perforation of the oesophagus, a necessary condition for the development of the specific complication which materialised, may be conditioned by it. The plaintiff had given evidence that if warned, she would have sought out the most skilled and experienced surgeon available.
The decision in Chappel v Hart suggests that the question of the relative skill and experience of the particular surgeon falls within the province of the law of negligence and not of battery. In Chappel v Hart that question was bound up with “the risks inherent in the [surgical] procedure” (at 276 [94]) and whether they had been disclosed, a matter undoubtedly relevant to negligence rather than battery. The pith of the law of negligence is bound up with questions about “the standard of care to be observed by a person with some specialist skill or competence.” All patients are entitled to expect that professionals engaged to provide services will exercise the ordinary skill and competence of the relevant profession. Questions of departure from the standard of care arise primarily in negligence and not necessarily at all in battery. Questions of whether a supervising surgeon ought to have known that a trainee had not yet acquired the relevant skill or competence expected in the profession, even under supervision, would likewise fall to be determined under the rubric of negligence and not battery.
If one posits an example where a patient consents to Dr A, a surgeon of ordinary skill and competence, performing an operation, who at the last minute and after the patient is under a general anaesthetic becomes unavailable, so that Dr B, also a surgeon of ordinary skill and competence, steps in, it could not, in my opinion, be said that that circumstance vitiates the plaintiff’s consent. The relevant consent is to the nature and character of the act. Papadimitropoulos demonstrates that the identity of the surgeon may be relevant to that question, however not in absolute terms, even though personal inviolability may suggest that those who can afford it have a right to choose their own surgeon. The real question, as the decisions in R v Richardson and R v Tabassum demonstrate, is about the requisite professional qualifications and here, as I have said, Dr Gundara was a legally qualified medical practitioner undergoing specialist training as a surgical registrar. He was to be supervised by Dr Payne in the performance of the surgery. Even if the express consent did not extend to that circumstance, adopting the broad approach approved in Rogers v Whittaker, I am of the view that the performance of the surgery by Dr Gundara did not alter the nature and character of the surgery so that Mrs Tinnock’s consent was vitiated.
Naturally the question of whether Dr Gundara’s performance of the surgery measured up to the standard of care to be expected from surgeons of ordinary skill and competence falls to be determined under the law of negligence. But I do not think an omission to obtain Mrs Tinnock’s express consent to the involvement of a doctor other than Dr Payne is a mistake on her part as to the nature and quality of the surgery to be performed.
In any event, for reasons I am about to give I am satisfied on the balance of probabilities that there was no omission to obtain Mrs Tinnock’s consent to the surgery being carried out by Dr Gundara under Dr Payne’s supervision.
Evidence concerning consent
It is logical to commence this discussion by pointing out that Mrs Tinnock, as is usual, signed a document headed “Consent form for medical procedure or treatment” on 25 February 2010 at the time of her first consultation with Dr Payne. The first part of the document was completed by Dr Payne and confirmed that he had provided advice on the nature of the treatment, likely results and material risks. The second part of the document was signed by Mrs Tinnock. It consists of 15 lines of printed information only. In substance it provides “I request and consent to the procedure/treatment described above for [me]”. That is a reference to the part of the form completed by the doctor which describes the proposed procedure as “incisional hernia repair (post-caesarian section)”. Among the printed matter in the section to be completed by the patient, at the twelfth line, is the following:
“I have been told that the procedure/treatment may be performed by another doctor.”
By asterisk the form provided for this line (and others not presently material) to be deleted “when not applicable” (Ex A, Vol 2, pp34-5). When cross-examined about the form (140.42-142.20 T) Mrs Tinnock identified her signature and agreed that she read the form although not word-for-word. She also agreed that her reading of it was “pretty close” to word-for-word. She agreed she had read the form “fairly closely” before she signed it. However she said she was unaware of the content of the twelfth line at the time she signed.
In her first evidentiary statement (Ex B1) Mrs Tinnock said she had been told about the incisional hernia after she underwent her third caesarean section on 2 October 2009. She consulted her general practitioner about the matter on 6 January 2010, underwent an ultrasound, and was referred to Dr Payne whom she first consulted, as I have said, on 25 February 2010.
She recalled that Dr Payne informed her that the hernia was large and that “he would use mesh in the repair” (Ex B1 [27]). She said “I understood Dr Payne would perform this surgery”. She also said (Ex B1 [29]):
“I have since become aware that that the surgery was performed by Dr Gundara and Dr Payne assisted.”
The statement does not otherwise deal with the issue of consent.
In his first statement of 9 April 2015 (Ex 9A) Dr Payne dealt with the circumstances of his first consultation with Mrs Tinnock in quite some detail. He said he had “some recollection” of that first consultation and it is clear that his recollection is supplemented by his specialised knowledge and his “standard practice”. As there is no issue concernig the information provided by Dr Payne about the nature and character of the procedure, it is sufficient to say that he explained his preferred approach in Mrs Tinnock’s case from among a number of available approaches. He also provided her with a copy of a brochure about the procedure published by the Royal Australasian College of Surgeons which is attached to his statement, which was open surgery utilising the “mesh plug method” (Ex 9A p34, see Ex L also). He said that as part of his standard practice he explained to patients that:
“In the public hospital system registrars are required to perform operations on public patients and the consultant surgeon will not always personally perform the procedure, so I tell my patients that a registrar may perform the procedure”.
Dr Payne said that he provided the consent form and obtained the plaintiff’s signature providing her consent.
Who performed the operation?
Dr Payne said that Dr Gundara performed the repair with mesh on 7 June 2010 and that he supervised “to ensure the procedure was conducted in an appropriate manner”. He assisted with “surgical instruments and retraction as required”. So much is clear from the operation record (Ex A, Vol 2, p49) which nominates Dr Gundara as the surgeon and Dr Payne as the assistant. In cross-examination (439.33-47 T) Dr Payne denied omitting to tell the plaintiff “that another doctor would or might be doing her operation”. It was clear, with respect, that Dr Payne was relying upon his standard practice. Again, he rejected the suggestion that he had not mentioned the role of registrars in the public hospital system. Again, he was relying upon his standard practice.
In his evidentiary statement of 22 January 2016 (Ex 12) Dr Gundara confirms being a legally qualified medical practitioner, and having become a Fellow of the Royal Australasian College of Surgeons in March 2015. He commenced his surgical training in 2008 and took up the position at Wagga Wagga Base Hospital as a registrar in general surgery in July 2009. As at the date of Mrs Tinnock’s surgery he was “approximately half way through [his] training program” (Ex 12 [4]). He did not have any independent recollection of seeing Mrs Tinnock before the surgery but it was his usual practice to introduce himself to patients before surgery. He said that it was not until the procedure commenced that he became aware of the part he would play. Both he and Dr Payne were “scrubbed in”. He acknowledged that he is designated in the records as the surgeon but his evidence is that both he and Dr Payne contributed to the performance of the surgery and “all relevant decisions about the surgery were made by Dr Payne” (Ex 12 [7]). His detailed account appears at [8]-[16] of his statement. It is unnecessary to set out the contents in full. From his account it is clear that Dr Payne was actively involved, directing Dr Gundara as to salient features of the procedure. His active involvement included placement of the mesh.
There was no relevant cross-examination of Dr Gundara about his description of the procedure followed during the surgery. He did accept, however, that he had no specific recollection of detailed events during the operation other than a vague recollection of the operation, assisted by the operation report (493.26-28 T). It was not, however, put to him that the matters relayed in the part of his statement to which I have referred were not accurate.
Mrs Tinnock’s supplementary statement
In her supplementary statement of 29 January 2016 (Ex B2) Mrs Tinnock was a little more expansive about matters surrounding consent which mostly took the form, however, of joining issue with Dr Payne on his statement about the matter. She denied any discussion about registrars performing operations in the public hospital system or receiving advice from Dr Payne that another doctor “might do [the] operation”. She did not consent to Dr Gundara operating; did not authorise Wagga Wagga Base Hospital “to choose who carried out the surgery”; and did not authorise Dr Payne to “choose who carried out the surgery”. Had she been told another doctor “would be doing the operation” she would want more information about their experience “and where Dr Payne would be”. She received no information on 7 June 2010 upon her admission that another doctor would be performing the operation and no-one introduced himself as “Dr Gundara”.
It was put to her in cross-examination that she had received the advice that Dr Payne said he had given in accordance with the standard practice. She denied receiving it (139.36-47 T).
Findings about consent
Reading the evidence as a whole, I am left with a very distinct impression that this is not a case where it can be said that Dr Gundara performed the operation rather than Dr Payne. Both Dr Gundara and Dr Payne were present and “scrubbed in”. Dr Payne was not merely standing by and watching. From Dr Gundara’s account, admittedly based largely on the operation note and his relatively faint recollection, Dr Payne directed Dr Gundara fairly closely as to what he was expected to do and took an active part in the procedures himself. I am satisfied that the operation was not done by Dr Gundara rather than Dr Payne. The reality was that the operation was performed by both doctors although Dr Gundara was the designated surgeon.
I appreciate that the evidence of both Dr Payne and Dr Gundara is very largely based upon matters of standard practice. However, this is common enough in cases involving professionals. Busy professionals have many cases and are unlikely to have a clear recollection of every detail of each case that may become significant years later when a dispute about what happened, refined by case management, goes to court. Evidence of standard practice is admissible circumstantial evidence of what happened on the particular day: Connor v Blacktown District Hospital (1971) 1 NSWLR 713 at 716 by Jacobs JA; at 721 by Asprey JA; (Mason JA agreeing); Bergman v Haertsch [2000] NSWSC 528 at [111], [271]; Peden v Ferguson [2012] NSWSC 492 at [117]-[118]; Smythe v Burgman (No 2) [2015] NSWSC 298 at [116]-[119]; and Tinnock v Murrumbidgee Local Health District (No 2) [2016] NSWSC 87.
Moreover the evidence of Dr Payne and Dr Gundara accords with what is generally known about the practice of surgeons, that is to say they very commonly work in pairs when performing surgery under general anaesthetic. For this reason, the evidence of Dr Payne and particularly Dr Gundara accords with what one might regard as the apparent logic of events.
Although it might be said that a patient like Mrs Tinnock to whom these matters are not routine might find them memorable, it is equally true that the significance of such details concerning the advice given about the involvement of registrars and the obtaining of consent lacked significance until she was questioned about them years later in the context of this legal proceeding. As they were likely to lack contemporaneous significance they were less likely to be memorable.
Moreover the document that she signed clearly states “that the procedure/treatment may be performed by another doctor”. The document is short, well-spaced and cast in plain English. As she read it fairly closely, pretty close to word-for-word, before she signed it, I am satisfied that she was aware of its contents and understood them when she signed it. This is not to say that she was lying when she gave evidence; to the contrary, simply that she has forgotten those details because she thought nothing of it at the time and accordingly they were not particularly memorable in the context of the information that Dr Payne gave her on 25 February 2010.
It had always been contemplated that Mrs Tinnock would be treated as a public patient. This circumstance is another factor which suggests that the probabilities favour the account given by Dr Payne of his usual practice. I am satisfied on the balance of probabilities that Dr Payne’s standard practice was followed on 25 February 2010.
Finally, Mrs Tinnock signed the consent form, which in form and content was clearly a legal document. As a unanimous High Court pointed out in Toll (FGCT) Pty Ltd v Alphapharm Pty Ltd (2004) 219 CLR 165; [2004] HCA 52 at 182 [47], the importance which the common law assigns to the act of signing a document is not limited to contractual documents, which in truth the consent form may have been. By reference to the improvident gift by deed in Wilton v Farnworth (1948) 76 CLR 646; [1948] HCA 20, bearing in mind that it was set aside on equitable grounds, the Justices explained (at 182 [47]):
“Legal instruments of various kinds take their efficacy from signature or execution. Such instruments are often signed by people who have not read and understood all their terms, but who are nevertheless committed to those terms by the act of signature or execution. It is that commitment which enables third parties to assume the legal efficacy of the instrument. To undermine that assumption would cause serious mischief.”
As I have said, there is no suggestion here of fraud or the like. I repeat that I am satisfied that Mrs Tinnock consented to the procedure and that her consent extended to the involvement of Dr Gundara as primary surgeon under the supervision of Dr Payne and with his assistance, as in fact occurred.
Section 3B Civil Liability Act 2002
The further amended statement of claim pleads reliance on s 3B of the Act. This pleading is intended to serve two purposes. First, to substantially circumvent the limiting provisions of the Act, in particular Part 2 concerning restrictions on personal injury damages. For instance, Mrs Tinnock claims aggravated and exemplary damages. The second purpose is to sidestep the difficulties which normally beset proof of negligence by surgeons.
By dint of s 3B(1)(a), the civil liability of a person in respect of an intentional act that is done by the person with intent to cause injury or death is excluded from the provisions of the Act. For the reasons explained by Leeming JA in Croucher v Cachia, absolving the Health District for liability in battery does not of itself exclude the operation of s 3B(1)(a): 67,636 [33]-[35]; see also Dean v Phung at 66, 339 [10]. Section 3B(1)(a) does not operate upon the particular cause of action “but instead upon the particular act which gives rise to the civil liability and the intent of the person doing that act”: Croucher v Cachia at 67,636 [33] [original emphasis]. Even though the alternative case is brought in negligence, the performance of surgery manifestly involves the performance of an intentional act, even if the matter said to constitute negligence consists of an omission like the failure to apply a negative pressure drain in this case.
In Department of Health & Community Services v JWB & SMB (“Marion’s Case”) (1992) 175 CLR 218; [1992] HCA 15, McHugh J (at 310[4]) said that the common law regards a surgical procedure as “usually [involving] the infliction of bodily harm on a patient”. Obviously dissecting the tissues with a scalpel involves “injury”, at least in the sense of inflicting harm or hurt. Thus a case could be made on a literal reading of s 3B that the performance of surgery (with or without consent) is “an intentional act done … with intent to cause injury”. However the matter is not free from authority. In Dean v Phung at 666,344 [30] Basten JA said:
”A medical procedure will generally be an intentional act: the critical issue is whether, in particular circumstances, it was done “with intent to cause injury”. In ordinary language, an injury is a harmful consequence. Something which is done with a therapeutic intent, that is, to prevent, remove or ameliorate a disability or pathological condition, would not ordinarily be so described.”
It will be otherwise where the surgeon knows when the surgery is performed “that the treatment is not reasonably necessary”. That is not so in this case. Although described as elective, there is no doubt that the surgery carried out was reasonably necessary treatment for Mrs Tinnock’s incisional hernia. Prior to the surgery her condition was continuing to worsen.
Accordingly, not because Mrs Tinnock has failed to establish battery, but because, even assuming negligence, the surgery was not done with intent to cause injury, s 3B(1)(a) is not engaged in the circumstances of this case.
THE PLAINTIFF’S ALTERNATIVE CASE IN NEGLIGENCE
As I have said above, Mrs Tinnock’s case in negligence is advanced by reference to alternatives.
Six medical specialists gave evidence on the liability issues. Five of them, the consultant surgeons, each provided separate reports to the solicitors qualifying; participated in the conference of experts and produced a joint report (13 February 2015, Exhibit J); and gave evidence concurrently. The five surgeons are Professor David Morris, Dr Geoffrey Miller, Dr Desmond Rea (plastic and reconstructive surgeon, see Tinnock v Murrumbidgee Local Health District (No 3) [2016] NSWSC 88), Dr Trevor Currer and Professor Christopher Berney. Of these, the reports of Dr Currer were served but not tendered as the defendant claimed legal professional privilege in respect of them. As he had participated in the experts’ conference and was a signatory to the joint report, I ruled that the plaintiff should be permitted to call him as a witness to give evidence concurrently: Tinnock v Murrumbidge Local Health District[2016] NSWSC 86. The sixth expert was Dr Tony Korman, a specialist in infectious diseases and microbiology. His report of 27 January 2016 is Exhibit K and was admitted over the objection of the defendant: Tinnock v Murrumbidge Local Health District [2016] NSWSC 86.
The open incisional hernia repair
The primary surgery (as described above at [34]-[35]) was carried out on 7 June 2010. The plaintiff’s case engaged the provisions of s 5B of the Act because it was said that Dr Payne and Dr Gundara were negligent in failing to take precautions against a risk of harm. The risk of harm was that which materialised being personal injury due to the post-surgical complication of infection “from an infected mesh”. The relevant precaution the plaintiff said should have been taken (which was not) was the use of negative pressure surgical drains.
All of the surgeons agreed that the infection suffered by Mrs Tinnock was a foreseeable and not insignificant risk arising from the open mesh incisional hernia repair carried out by Dr Payne (327.4-20 T).
The real issues relate to whether a reasonable surgeon in the position of Dr Payne would have taken this precaution, that is to say, whether the standard of care of a surgeon of ordinary skill and competence required the use of drains on the particular occasion of Mrs Tinnock’s surgery.
The remaining issue is whether taking the precaution would have avoided the infection.
Was the use of negative pressure drains required by competent surgical professional practice in the circumstances of the case?
I think it important to point out there were factors personal to Mrs Tinnock which enhanced the known risk of post-surgical infection. They were:
She was a smoker who had been unable to give up during the period of surgery and recuperation. Smoking increases the risk of infection because it slows the healing process, extending the opportunity for infection to intrude (361.10-362.13 T);
She was obese, having a body mass index of 34 (362.19 T). The fatty tissue is very high in calories, is warm and humid, and has a poor blood supply. As Professor Berney said, “bugs love this place” (363.8 T); and
The site of the previous caesarean incision was very low in the abdomen. Dr Currer said “this is the worst possible site for operating to avoid an infection” (362.27-28 T).
This combination of risk factors was well recognised by surgeons in 2010 (364.6 T).
These three factors significantly enhanced the risk of infection. Dr Currer said, “those three factors are massive” (362.42 T). He also said (362.34-40 T):
“… this case is a nightmare, if I may say, for a surgeon … it is not an easy case. This patient was waiting for an infection. This was on the cards right at the outset.”
It was also recognised by surgeons in 2010 that because mesh repairs by definition involve the placement of a, albeit prosthetic, foreign body deep in the patient’s abdomen, the risk of infection is further enhanced. This particular risk has been reduced by the introduction of a newer generation of surgical mesh with larger pores such as Dr Payne used in Mrs Tinnock’s case. Even so, Dr Currer said, “once there is a mesh in place, if you suspect infection, you consider the mesh is implicated” (322.21-22 T). A third circumstance that needs to be borne in mind is the distinction between a seroma and an infection. A seroma is a collection of serous fluid produced as a reaction to inflammation to the trauma that has been done to the body by the surgery (329.44-45 T). Professor Berney was of the view that “seromas are a normal outcome from hernia repair” (314.9-10 T). Dr Currer agreed that every operation of the nature undergone by Mrs Tinnock “will have some degree of seroma” (314.3-4 T). I understood those views to represent a consensus of opinion. All of the surgeons agreed that the development of a seroma does not indicate that surgery was performed in a manner which did not accord with competent professional practice (Ex J, [6]).
All of the surgeons also agreed that the development of a post-surgical infection was not evidence that surgery was not performed in a manner falling short of competent professional practice (Ex J, [7]).
An infection may develop independently of the development of a seroma and whether or not a seroma occurs. All of the surgeons agreed that a seroma may “provide a substrate” for infection (Ex J, [4]). Dr Currer expanded on what is meant by a substrate. He explained that a seroma can form a culture medium which may enhance bacterial growth (349.35-6 T). Further, he said (313.49-314.4 T):
“Usually infections of a wound of this nature start at the time of the first operation. Whether there was a seroma or not may have had no influence whatsoever. If there was a seroma it may aggravate the infection but an infection can occur without a seroma and [it’s] preferable not have a seroma but, having said that, every wound or incision of operation of this nature will have some degree of seroma.”
It was common ground “that you can have a seroma that is not infected” (314.21-22 T).
Under Dr Payne’s supervision and with his assistance, Dr Gundara did take precautions to reduce the risk of infection. Naturally the surgery was carried out in the sterile environment of the operating theatre. But more specifically, all of the layers cut open to access the area of the hernia were closed by sutures, pressure dressings were applied, and post-surgically an abdominal binder (like a surgical corset or girdle) was prescribed. Prophylactic antibiotics were also prescribed (Ex J [53]). These steps are described in more detail at [34]-[35] of Exhibit 9A, Dr Payne’s first evidentiary statement. The main purpose of the methodology adopted was to promote adherence of “the mesh to the plaintiff’s fat and muscles and eliminate dead space” (Exhibit 9A [35]). Dr Payne said that decreasing the dead space reduced the subsequent risk of infection (Ex 9A [38]).
In his statement of 22 January 2016 (Ex 12), Dr Gundara described dissecting three layers being the skin, the dermis, and the fatty tissue, to gain access to the hernia. It was then necessary to dissect the sac away from the underlying subcutaneous tissue. The hernia sac was pushed through the defect which was then closed with sutures. The mesh, which was quite large in this case, being 25cm x 12cm, was then placed over the imbricated sac. The mesh was fixed in place with eight Prolene sutures and forty tacks (Ex 9A [34]). The fatty tissue layer was then sutured over the mesh “in order to minimise dead space” (Ex 12 [16]) and the dermis and skin layers were closed with sutures. Pressure dressings held in place by adhesive dressing were applied over the wound, again “to minimise any dead space” (Ex 12 [18]).
The consultant surgeons agreed that all of these steps were consistent with competent professional practice. The debate concerned whether a surgical drain was also required.
Dr Miller was adamant that drainage was “mandatory” (Ex J [53], [66]). The basis of Dr Miller’s view was that the size of the mesh prosthesis militated against the elimination of the so-called “dead space”. To put it positively, he did not believe the dead space could be adequately closed by the measures adopted by Dr Payne (Ex J, p 3 [8], p 4 [13]).
Professor Morris was also of the view that the failure to employ drains “represented a departure from competent professional practice” (Ex J, [64]). Dr Rea was of the view that the question depended upon whether, despite the measures already adopted, “there was a significant dead space” (Ex J, [64]).
In the joint report, Professor Berney and Dr Currer expressed the opinion that the failure to employ drains in the present case did not represent a departure from competent professional practice (Ex J [64]).
My understanding of the evidence of all of the experts is that competent professional practice does not require the closure of all open abdominal surgery with drains. On the other hand, all agreed that drains are required in certain cases. The difficulty was eliciting what circumstances called for the use of a drain.
Dr Miller said that suction drains are commonly employed by all of his peers and he called them “a closed system” (328.33 T). He said that it is his practice “to put one to two drains in the large dead space … to further decrease the risk of … seroma” (328.15-16 T). He described the process in this way (328.33-43 T):
“So, the area where the drain penetrates the skin can be fastidiously cared for to avoid infection and what the drain does is it removes, first of all, any blood and serum that may accumulate as a result of the initial operation and what it does is also promote the adherence of the overlying subcutaneous fat to the underlying fascia, in other words, eliminating the defect and bringing the two layers together and, in doing that, promotes wound healing and also aids in the reformation of the lymphatics that have been disrupted by the surgery to find new pathways such that the fluid that they are producing doesn’t accumulate in the wound, but actually finds its way back into the body through another portal.”
The other side of the argument was perhaps put best by Professor Berney. He said (329.5-8 T):
“Putting a drain or not putting a drain is not right or wrong. I sometimes put [a] drain; sometimes I don’t put [a] drain. A drain, importantly, is to make sure, first of all, there is no bleeding, control of any bleeding, because if you have bleeding then the risk of infection is much higher.”
He went on to describe the drain as a personal choice within the judgment of the surgeon. I formed the impression that that judgment related to this question of the dead space because he said “there may be other ways to reduce the seroma” (329.25 T).
In Dr Payne’s opinion (Ex 9A [36]):
“The use of a drain is required where there is bleeding or infection; in the plaintiff’s case, neither was evident so the use of a drain was not required. In the absence of any bleeding or infection, and in circumstances where Dr Gundara had achieved good attachment of the mesh to the plaintiff’s fat and muscle thereby eliminating any dead space, inserting a drain would have been a conduit for infection and this was heightened in the plaintiff’s case as the drain would have had to be inserted into her groin region.”
It is apparent that Dr Payne sees a role for drains in open abdominal surgery. I found it difficult to understand the reference to infection given that he was not treating Mrs Tinnock, certainly at that time, for a condition involving infection. It is also curious that he did not regard the control of a seroma as a relevant consideration when all other surgeons did, at least where dead space was likely. I accept he expressed a view that he was satisfied the dead space had been eliminated, at least at the conclusion of the surgery on 7 June 2010.
Each of the surgeons recognised that a drain may be a portal for the introduction of infection: eg Dr Currer (Ex J p6 [4]); Professor Berney (329.14-15 T). But none of the consultant surgeons were of the view that it was necessary to position the drain near or into the groin region (334.2-21 T). Dr Miller explained, “because it is a negative pressure drain, you can place it at the top of the wound … because it is going to function on negative pressure not on dependent drainage”.
The risk of infection from the drain relates to the length of time for which the drain is left in place. It is obvious from the evidence of the experts that a relatively short time is preferable. Dr Currer was reluctant to leave it in for more than 24 hours. Dr Miller said that it could be left in for between 10 days to two weeks (330.6-7 T). Professor Berney said if a drain is left “too long” the risk of infection from the drain increases drastically (329.14-15 T).
Dr Currer said “it is customary to drain after a large mesh repair but not obligatory” (330.29-30 T). He also said (330.38-40 T):
“I always drain these big ones, often with four big closed system drains but the surgeon felt he had adequately closed this and that may well be the case”.
Dr Rea thought, “it is prudent and almost obligatory” to drain (330.45-46 T). Professor Morris agreed that a drain should have been used.
While agreeing that a judgment had to be made at surgery, Dr Currer said (338.31-44 T):
“It depends on the size of the repair and extent of the subcutaneous dissection required and it also depends on how the mesh is put in and the closure that is done.
…
His Honour: In your opinion … this was big enough to justify a drain?
Dr Currer: Definitely and especially a superficial mesh, superficial to the muscle, deep to the muscle layer, perhaps one would be able to avoid it”
I took the latter comment to mean that Dr Currer was doubtful that it could be avoided.
Findings about the use of surgical drains
Although there was no universal practice in June 2010 that surgical drains should be employed in a case such as Mrs Tinnock’s, I accept that there was “wide acceptance” that a drain (or more than one) should be used (335.5-27 T). I was left with the distinct impression that although there was a natural reluctance on the part of some of the experts (especially Professor Berney and Dr Currer) to criticise their colleague, each of the experts giving evidence would have used a drain in this case. All were doubtful of whether sufficient closure of the so-called dead space could be achieved in such a case. Moreover, given the particular risks attending this case as discussed above, a drain or drains was, or were, called for.
I was not, with respect, impressed with the views strongly put particularly by Professor Berney that it was in the end a matter solely for the surgeon’s discretion. I appreciate that surgery will not necessarily involve following a textbook and that decisions will have to be made on the spot. At the same time, the factors informing the decision about whether a drain should have been used clearly pointed to this case being an appropriate one. Moreover, Dr Payne’s explanation for not using one was, to say the least, somewhat out of step with the views of the experts.
I appreciate that the question of what ordinary skill and competence requires of a consultant general surgeon is not adjudged by either the balance of expert opinion called in the case, or according to the sum of its parts. Even so, the court has to be guided by the opinions of the experts actually called to give evidence.
I am not persuaded by the view that the decision is solely within the discretion of the surgeon is a complete answer to a case in negligence because even the best professional can make an avoidable mistake. Moreover, to say the question is to be determined in the surgeon’s sole discretion is to treat the use of surgical drains as though they were an optional extra when the evidence clearly indicates that they have a therapeutic role to play, including in reducing the risk of infection, admittedly in conjunction with the other matters I have referred to.
I am of the view that the standard of care to be observed by the surgeon of ordinary skill and competence required the use of negative pressure surgical drains in a case as complex as Mrs Tinnock’s.
Conclusion about breach of duty
Turning then to the provisions of s 5B of the Act, I am satisfied that the risk of harm to Mrs Tinnock which materialised in this case was both foreseeable and not insignificant. In the circumstances, a reasonable surgeon in Dr Payne’s position would have taken the precaution of employing negative pressure surgical drains. In deciding that a reasonable surgeon would have taken that precaution, I have considered the matters set out in s 5B(2) of the Act. The probability that harm will occur if care were not taken is not necessarily high, but given that infection is a known risk, it was not one that should be disregarded. The type of harm which could eventuate was known to the medical profession as potentially grave. The burden of taking the precaution of utilising drains in addition to the other precautions taken by Dr Payne was slight. On the evidence of the experts I infer that these drains are relatively cheap and readily available. Indeed, given that they are not always obligatory and the surgeon can exercise a discretion, I would infer they are readily available in the operating theatre. Medicine, of course, is of the highest social utility, but only when practised with reasonable care. I am satisfied that the Health Area is vicariously liable for the omissions of Dr Payne and breached the duty of care it owed to Mrs Tinnock.
The second procedure of 15 June 2010
As I have said already, the plaintiff presses further grounds of negligence in the performance of each of the second and the third procedures. It is important to bear in mind, however, that Mrs Tinnock’s various presentations to the hospital, and the findings made, are separately relevant to the question of causation; although, frankly, it is hard to see there being any serious question about the infection with which she presented to Calvary Hospital, Canberra, on 17 July 2010 being a direct consequence of the surgery of 7 June 2010. Indeed, no one said otherwise. The experts differed as to when the infection arose and when it was reasonably detectable by a medical practitioner, not necessarily the same thing. It seems to me that those matters are only material to the question of whether the treatment provided in the meantime measured up to the relevant standard of care. There may be an intermediate causation question. For instance, if I am not persuaded that the use of drains in the surgery of 7 June 2010 would have made any difference to the outcome, what about the second and third procedures? Should they have been approached differently leading to a different outcome and so avoiding the much more serious consequences that had befallen Mrs Tinnock by 17 July 2010?
In the final analysis, all of these issues reduce to a single question: should Dr Payne have diagnosed an infection and removed the mesh at the time of the second or third procedure? If so, would Mrs Tinnock’s injuries have been measurably or appreciably less severe? As I have said, these matters really only arise if Mrs Tinnock’s injuries were not caused by negligence during the first procedure.
At the time of her discharge following the open repair on 9 June 2010, it was Dr Payne’s expectation that the plaintiff could be followed up by her general practitioner if necessary as the sutures in her abdomen were of the dissolving type. It ought not to have been necessary for her to be reviewed by a specialist for a further four to six weeks, as he indicated. However, the plaintiff re-presented to the hospital on 13 June 2010, only six days after surgery. The diagnosis made was of a seroma following her incisional hernia repair.
Mrs Tinnock asserted that a resident medical officer commented to her, “it is most likely infected but we won’t remove the mesh” to which she responded, “If it’s infected get it out” (Ex B1 [32]). I am not satisfied that such an exchange occurred. It seems most unlikely that a resident medical officer would have had insufficient information at the point of admission to make such a comment, let alone the expertise. As I hope I have made clear, infected mesh certainly became the diagnosis as she must be aware and I think it probable that Mrs Tinnock has conflated different information she received at different times.
Mrs Tinnock’s symptoms on presentation on 13 June were “oozing and bleeding” from the wound with associated abdominal pain. Mrs Tinnock described the fluid as “orange-red” with “an offensive odour” (Ex B1 [33]). She complained of nausea and loss of appetite. No fever was recorded upon presentation. She had completed the course of an oral antibiotic, Keflex, with which she had been discharged. On examination she was mildly tender around the wound which was discharging but there was no dehiscence, or breakdown, of the surgical wound itself. The impression of Dr Gamble, the consultant general surgeon on call who examined her, was that she had a mild wound infection six days post-operatively. She was admitted and commenced on a course of strong intravenous antibiotics. Dr Gamble thought it likely that she would require an ultrasound-guided surgical drainage.
A Dr Burnton examined Mrs Tinnock on 14 June 2010 and formed the impression that she suffered a “wound infection/collection following incisional hernia repair”. Dr Gamble examined her later the same day and noticed a “large amount of discharge from the wound”. He recorded in the hospital notes (Ex A Volume 2 p86) a large amount of discharging brown fluid and secondary erythema, or redness, of the skin. A culture swab of the discharging wound was taken and sent for pathology and an absorbent dressing applied.
I interpolate on 15 June 2010 (Ex A, Volume 2, [87]) Mrs Tinnock complained of the sudden onset of lower back pain while in hospital.
Mrs Tinnock was examined by Dr Payne on 15 June 2010 who decided that it was appropriate to undertake a “washout, exploration of Mrs Tinnock’s abdominal wound and application of VAC dressing” (Ex 9AB [54]; Ex A, Volume 2, [87]). At surgery Dr Payne found a “large cavity above the mesh with the wound opening infra-umbilically”. The seroma was drained by suction and the VAC dressing was applied. In his evidential statement (Ex 9A [57]) Dr Payne said:
“There was no indication the plaintiff was septic and there was no abdominal cellulitis or physical evidence of infection.” [Original emphasis]
The wound swab that had been taken by Dr Gamble indicated mixed anaerobes which Dr Payne regarded as “normal skin flora, not infection”. No swab was taken during surgery from the mesh or otherwise deep in the abdomen.
Mrs Tinnock was discharged on 18 June 2010 with a “minivac” dressing which would require changing by community nurses. She was to be seen at the outpatients’ clinic on 24 June 2010.
A junior medical officer who accompanied Dr Payne and a registrar, Dr Chen, on their ward round on 18 June 2010 before Mrs Tinnock’s discharge acting as “scribe” (422.34T) made a record including the matter, “Infected seroma improving with IVAB and VAC dressing” (Ex A V2 p 94). IVAB means intravenous antibiotics. The entry is signed by Dr Celeste Vidot. Dr Payne took issue with the reference to “infected seroma”. He could not recall the medical officer but said in his statement that the entry “ha[d] been written in error” (Ex 9A [66]). He was carefully cross-examined about this topic at 422.25-424.15T. He maintained the note did not record accurately what he had said, although he agreed he would have had occasion to review it more than once and I infer did not see fit to alter it. The note is detailed and written in a careful hand. Other examples of Dr Vidot’s record-keeping are in evidence and she is obviously meticulous. I am not of the view that the relevant entry was recorded “hurriedly” (423.9T). I have the impression that Dr Vidot accurately recorded what was said.
Dr Vidot also completed the discharge summary for that admission (Ex A, Volume 2,p74). She made a very careful record of Mrs Tinnock’s presentation, procedures carried out and the results of relevant investigations including the consideration that the wound swab had shown “mixed anaerobes +++”. She made no express reference to “infection” in this document, notwithstanding the printed part of the form made reference to “additional diagnoses/complications/infections (comorbidities/complications affecting patient care)”.
A lot of forensic effort was put into proving that from 13 June 2010 Mrs Tinnock was suffering from an infection which ought to have been picked up by Dr Payne. There was a great deal of picking over the contents of the clinical notes for signs of infection. For instance, at Exhibit A Volume 2 p 77, when first examined after being triaged, there are references to querying whether the fluid oozing from Mrs Tinnock’s wound was pus. Emphasis was placed upon various uses of the participle “infected” in places including in Dr Vidot’s note and a possibility raised by the radiologist who took a CT scan of the collection (Ex A V2 p 96).
Dr Korman’s report was relied upon in this regard. I think it can be said that Dr Korman was of the view that although some of Mrs Tinnock’s signs and symptoms on presentation might be explicable by reference to a seroma alone he thought it more likely than not that there was “an infected seroma and/or wound infection” (Ex A Volume 1 p 153). He relied upon: oozing from the wound; the fact that wound infection elevated white cell count; elevated neutrophil count; elevated platelet; count elevated C-reactive protein; wound swab microscopy results; the size of the fluid collection; the erythema (inflammation); the discharge of brown fluid; and the treatment administered including drainage and intravenous antibiotics. He was of the view that that treatment was not consistent with prophylaxis. Indeed Dr Vidot’s note of the ward round of 18 June indicates a professional impression on the part of Dr Payne that the “infected seroma” was improving with heavy duty antibiotics and the use of the VAC dressing (or pump or drain). This suggest too suggests treatment for infection and not prophylaxis.
Dr Payne maintained that use of a VAC dressing was contra-indicated in the case of infection (428.35-6T). However he agreed that the material produced by the hospital concerning its use included use for infected Caesarean section wounds (429.7-10T; Ex A V2 p 189). As I have recorded elsewhere Mrs Tinnock was treated by use of a VAC dressing for some months following her surgery at Calvary Hospital to address what was found to be a massive mesh infection. This too sits uneasily with Dr Payne’s assertion. I think Dr payne is mistaken in his assertion.
It is evident that there may be different degrees of infection. It seems clear to me that Dr Payne is referring to a major infection presenting as sepsis. I do not understand his evidence to exclude the possibility of a lower grade infection at that time. Indeed the only way can understand all of this evidence as a whole is that he was concerned about infection at that time and was treating it even if there was no overt evidence of sepsis or the like.
Professor Berney was firmly of the view that there was no objective evidence consistent with established infection at least until the middle of July 2010. Dr Currer’s view was that the infection was probably introduced at the time of the original procedure on 7 June 2010, and Dr Miller was of the view that the infection was probably introduced when the wound around the umbilicus opened, permitting the discharge of the fluid. He made the distinction between someone with septicaemia and the lesser infection (319.40 T). Professor Morris thought there was clear evidence of infection (321.30 T). Dr Rea was unable to express a view because he had not closely considered all of the clinical material from Wagga Wagga Base Hospital.
Although Dr Currer was of the view that “there was not absolute proof of infection” (321.47-8 T) he also said (322.10-15 T):
“… I’m sure we agree – there is an overlap of agreement here that you can have degrees of infection and an overt infection with pus, that would be an abscess, but you can have low grade forms of infection which can be the beginning of infection which may have very subtle clinical signs and biochemical parameters and one needs to latch onto that and treat it aggressively and that’s what was done.” (my emphasis)
He also said, I repeat, that if you suspect infection you consider the mesh is implicated (322.21-22 T).
I accept on the balance of probabilities there was probably the type of low grade infection that Dr Currer referred to present at the time of Mrs Tinnock’s presentation on 13 June 2010. There was no suggestion then of septicaemia. But Dr Payne’s denials of infection of any kind at that time (or indeed at any time when Mrs Tinnock was under his care) cannot be accepted. However, I am not persuaded that Dr Payne should have done anything different in his procedure on 15 June 2010. Professor Berney said with modern meshes one attempts to keep the mesh. He pointed out that Dr Payne did put in a drainage system (the VAC dressing) which was the correct approach (339.19-21 T).
Dr Currer agreed that the management of the second surgery was appropriate. He said (339.25-29 T):
“… it was [un]necessary to remove the mesh at that time. The modern day meshes – there’s been enormous progress and changes in the meshes over the period of 35 to 40 years. The modern day meshes are resistant to low grade infections.”
Dr Rea agreed with Dr Currer’s conclusions. Dr Miller said the second operation was quite appropriate (339.36-42 T).
Three things are said about breach of duty at this time, essentially. First, that a swab from deep in the wound should have been taken; secondly, that possibly the mesh should have been removed and thoroughly washed if it was to be retained; and thirdly, that perhaps a long period, say a month, of intravenous antibiotics should have been instituted.
It probably would have been advisable to take a culture from the wound given the signs of low grade infection but in the end I am not satisfied that the treatment would have been any different. Removing the mesh either permanently or to wash it with topical antibiotics (Professor Morris at 348.1-4 T) would have undone the previous surgery which was reasonably necessary treatment for the incisional hernia very soon after its performance. A course of intravenous antibiotics was given over a period of days. Admittedly using hindsight, even when the infection became critical no-one instituted a course of intravenous antibiotic treatment for as long as one month. I am not satisfied that there was any breach of duty by Dr Payne (or anyone else for whom the defendant was vicariously liable) in respect of the second procedure.
Subsequent progress and the procedure of 27 June 2010
Mrs Tinnock was examined by Dr Chen, surgical registrar, on 24 June 2010 in the outpatients’ clinic, but nothing concerning was discovered (Ex A V2 p 1).
She was readmitted to Wagga Wagga Base Hospital on 27 June 2010 for the delayed closure of her abdominal wound. She had been in the meantime using the minivac machine and had been attended by a community nurse every second day. Mrs Tinnock said the community nurse told her on 27 June 2010 that there was a lump in her abdomen and she needed to attend the emergency department (Ex B1 [38]). This account was challenged in cross-examination (148.38-48T) but Mrs Tinnock’s account is corroborated by the Wagga Wagga Base Hospital clinical notes (Ex AV2 [147]). It is apparent that she attended the emergency department on 27 June 2010 on referral from the community nurse. The complaint is recorded as: “has noticed lump under suture line”. The notes record that the VAC dressing had ceased until “further orders post-medical [review]”.
As things transpired, Mrs Tinnock was examined by Dr Payne in the emergency department. He recorded that Mrs Tinnock’s hernia repair had been complicated by a seroma leak. On his review he assessed the wound to be “clean with no evidence of infection”. His note also records that Mrs Tinnock was keen to have the wound closed. I am prepared to accept that this is correct, given the difficulties she had suffered since the original surgery. In his statement (Ex 9B [69]), Dr Payne said there was nothing about Mrs Tinnock’s presentation that caused him any concern. I infer he means concern about infection, for he says had he been concerned, he “would not have agreed to close her wound”. Professor Berney commented that “no surgeon will close a wound if [there] was obvious infection” (315.44-45 T).
Dr Payne recorded his operation findings in these terms (Ex A V2 p 166): “Cavity overlaying mesh, no pus / abscess cavity granulating edges of skin”.
Antibiotics were again prescribed, Dr Payne says as a prophylaxis (Ex 9A [75]). Mrs Tinnock was discharged on 28 June 2010. The discharge summary was again completed by Dr Vidot (Ex AV2 [145]). Dr Vidot wrote under “Presentation”:
“39 year old female patient presented for delayed closure of abdominal wound. She had a repair of a ventral (mesh) hernia and represented 10 days later with an infected wound seroma.
I take the reference to the infected wound seroma to be a reference to the admission of 13 June. Dr Vidot also recorded that “nil pus or abscess cavity was identified”. This latter entry in terms relates to the closure procedure on 27 June 2010.
I accept that there was no overt sign of infection at surgery. However, I accept that notwithstanding the treatment she had had, including antibiotics and VAC drainage since 13 June 2010, a low grade surgical infection continued to be present, the signs of which were not visible to the trained eye.
The plaintiff was discharged on 28 June and re-examined at the outpatients’ clinic on 1 July 2010 by Dr Chen (Ex A V2 p 2). The wound was found to be clean and was redressed.
Mrs Tinnock attended the hospital again on 3 July 2010 when she was re-admitted until 5 July 2010. Initially, she was seen by Dr Gundara in the emergency department who recorded “wound complication” (Ex AV2 p 194). He noted the review by Dr Chen “three days ago” and queried whether there was an issue then. (None was recorded by Dr Chen.) He received a history of an increase in swelling and pain around the wound and bleeding. Mrs Tinnock complained of associated nausea and fever. On examination he found erythema around the wound and a “serous / bloody / purulent discharge”. Among his impressions were wound dehiscence with “? – collection / infection”. He recorded that he was “alert to possibility of infected mesh”.
Dr Gundara admitted the patient to be reviewed by Dr Payne. It is clear from the clinical notes (Ex AV2 p 193), but not from Dr Payne’s statement, that Mrs Tinnock was very upset when she saw Dr Payne in the emergency department. There seems to have been a contretemps. However, on examination he noted “old blood on dressing” and questioned whether it was haematuria.
It is clear that at this time Mrs Tinnock and her family were not happy with the treatment they were receiving at Wagga Wagga Base Hospital. The notes record that Mrs Tinnock’s mother rang the emergency department on the same day to volubly complain about the treatment her daughter was receiving.
Dr Payne’s notes of his review of Mrs Tinnock on 4 July 2010 (Ex AV2 p 203) are difficult to read. In his statement he says the white cell count was normal. He ordered antibiotics and the redressing of the wound. A raised white cell count would be consistent with sepsis (Ex 9A p 81). She continued to be treated with intravenous antibiotics. On review on 5 July the wound continued to ooze mildly. Dr Payne felt Mrs Tinnock could go home with community nursing support and the avoidance of heavy lifting. At discharge the nursing sister recorded “no ooze, nil signs of infection, some skin irritation on sides” (Ex AV2 p 205). The discharge summary was again written by Dr Vidot who seems to have been present on Dr Payne’s ward round on 5 July 2010 because her distinctive neat handwriting completed the marginal note. She recorded the diagnosis as wound dehiscence. She recorded the presentation as a one to two day history of wound redness and swelling including discharge of haemo-serous fluid which improved with intravenous antibiotics and daily wound dressings. Mrs Tinnock was to be followed up by the surgical registrar three days later. As it transpired, she was unable to attend on 8 July 2010 because she was too unwell.
I am satisfied on the balance of probabilities that when she presented on 3 July 2010 the plaintiff was suffering from obvious signs of wound infection as recorded by Dr Gundara. That Dr Payne took a more robust view does not dissuade me from this conclusion. Apart from anything else, it is quite clear that the doctor patient relationship had broken down at that stage and this may have affected his perception. In accordance with Dr Gundara’s impression, serious questions should have been asked by Dr Payne about the real possibility of mesh infection requiring aggressive treatment including re-exploration of the wound (as occurred at Calvary Hospital). At that time it would have been appropriate to adopt Professor Morris’s suggestion of washing the mesh with topical antibiotics, and commencing a prolonged course of intravenous antibiotics beyond the three day course in fact provided, at least if it was considered the mesh could be “saved”.
Dr Payne tended to put the obvious “complications” with which Mrs Tinnock presented on 3 July 2010 down to her obesity and smoking (Ex 9A [80]; 246.13-247.21 T). However, as he agreed, they were known risk factors requiring extra care and attention (246.30 T). This does not explain his continual resort to “IVAB”.
I am persuaded that Mrs Tinnock’s presentation then was due to mesh infection and not delayed healing due to her obesity and smoking. But I am not satisfied that Dr Payne should not have carried out the delayed abdominal closure on 27 June 2010. I can well understand that Mrs Tinnock was keen to be rid of the VAC drain and to bring this long course of treatment to an end. More importantly, I accept the reliability of Dr Payne’s observations that there were no overt signs of serious infection which would have precluded closure. I am not persuaded that surgical drains should have been utilised at the third surgery. I accept that fluid accumulation may have been a continuing issue and that drains “may have a role to play” (244.28-30 T). I accept Dr Payne’s evidence that the cavity referred to at the third operation on 27 June 2010 was referrable to “the small incision previously occupied by the VAC foam”. This was a smaller area than that previously occupied by the seroma (244.36-41 T).
However, I repeat that although there were no overt signs of serious infection such as sepsis on 15 June 2010, Dr Gundara’s findings strongly suggest that had changed by 3 July 2010. I am satisfied that there were signs initially of a low grade infection and eventually of a serious infection, the latter by 3 July 2010 whilst Mrs Tinnock was under Dr Payne’s care, contrary to his evidence (426.47-427.2 T).
Mrs Tinnock kept her appointment at the outpatient clinic on 15 July 2010 and was examined by Dr Chen. Dr Chen found “a leaking abdominal seroma” and “6x6cm area of skin necrosis”. His plan was to admit Mrs Tinnock for yet more intravenous antibiotics, surgical debridement of tissue and drainage of the “seroma”. He discussed the plan with Dr Payne who agreed with it (Ex AV2 [3]). Considering the material as a whole and particularly bearing in mind Dr Gundara’s findings on 3 July 2010, I am persuaded that Dr Chen was recording evidence of infection. Indeed his first treatment proposal was more intravenous antibiotics. This would have been the third occasion on which that treatment had been instituted. Mrs Tinnock received intravenous antibiotics when she was admitted on 13 June and 3 July 2010. I do not accept that this was mere prophylaxis. Indeed Dr Korman made very clear the very limited role of antibiotics as a prophylactic for infection. He was strongly of the view that this course of treatment was only appropriate to treat infection (391.27-392.15T; 399.25-27T).
Dr Payne maintained in evidence that Dr Chen’s findings at 15 July 2010 did not suggest infection (443.35 T). He continued to put clinical signs down to Mrs Tinnock’s smoking. He said that had there been an infection at that time he would have expected to see other features such as cellulitis, an infection of the skin. It is important to bear in mind that this is just 24 hours before Mrs Tinnock was admitted to Calvary Hospital, Canberra, with what all the experts agree was a massive mesh infection requiring urgent and radical treatment, including removal of the mesh.
When questioned about Dr Gundara’s note of 3 July 2010 (355.20-358.47 T), all of the surgeons other than Professor Berney were of the view that the clinical signs were then consistent with an infection deeper in the wound and consistent with “an overt mesh infection at that stage” (Dr Currer 358.35 T). Professor Berney accepted that if the discharge was purulent (“there was a wound infection”, 356.25 T) but “there was no clear sign of infected mesh there” (359.31 T).
I find Professor Berney’s opinion unpersuasive. At surgery on 17 July 2010, only two days after Dr Chen wanted to readmit Mrs Tinnock, a large cavity of necrotic tissue was found with the mesh on view. It is hard to conclude that that situation came up overnight after Mrs Tinnock decided not to be re-admitted to Wagga Wagga Base Hospital but to go to Canberra instead (Ex AV2 p 271). It is also notable that upon examination at Calvary Hospital, Canberra at 1.40am on 16 July 2010 the clinical impression of the emergency department registrar was that she was suffering from an ongoing post-operative wound infection with an underlying collection (Ex A V2p 253). At that time her temperature was 37.8 degrees after ingestion of panadeine forte. That these findings were made then strongly supports the idea that she was misdiagnosed at Wagga Wagga Base Hospital.
As I have said, I am persuaded that by 3 July 2010 there were overt signs of infection. The infection improved in response to intravenous antibiotics from time to time but it did not clear up because the ongoing source of the infection remain within Mrs Tinnock’s abdomen, that is to say the surgical mesh. As Dr Currer said, if there are signs of infection, suspect the mesh; just as Dr Gundara did.
Conclusions about liability
In my judgement, Dr Payne’s care of Mrs Tinnock fell short of the standard of the surgeon of ordinary skill and competence in two respects. The first was in failing to use negative pressure drains in the original repair of the incisional hernia; and the second was in failing to identify the mesh infection by 3 July 2010 and failing to treat it much more aggressively by re-operating to remove the mesh for washing with topical antibiotics if he thought it could still be saved or simply removing it all together.
Legal causation
Questions of causation are to be determined in accordance with the provisions of ss 5D and 5E of the Act. The plaintiff always bears the onus of proving on the balance of probabilities any fact relevant to the issue of causation. The determination of causation is comprised of two elements. The first is that the negligence is a necessary condition of the occurrence of the harm. This involves the application of the “but for” test: Adeels Palace Pty Ltd v Moubarak (2009) 239 CLR 420; [2009] HCA 48. The second is that it is appropriate for the scope of the negligent person’s liability to extend to the harm so caused.
In an established category of duty of care, like the duty owed by a surgeon to a patient, the second question will rarely provide any difficulty. Generally it will be appropriate, according to the normative standards which underpin negligence law, for the surgeon’s liability to extend to the injury caused by the negligence: Wallace v Kam (2013) 250 CLR 375; [2003] HCA 19 at 385 [21]-[22]. It will be otherwise in novel cases: Wallace v Kam at 385 [23]; see also Paul v Cooke (2013) 85 NSWLR 167; [2013] NSWCA 311.
As Hayne and Bell JJ pointed out in Tabet v Gett (2010) 240 CLR 537; [2010] HCA 12 at 564 [66], in a medical negligence case, what the plaintiff must demonstrate on the balance of probabilities is that the defendant’s negligence was a cause of a detrimental difference to the plaintiff. Their Honours said at [66]:
“The comparison invoked by reference to “difference” is between the relevant state of affairs as they existed after the negligent act or omission, and the state of affairs that would have existed had the negligent act or omission not occurred.” [original emphasis; footnote omitted]
I am satisfied on the balance of probabilities that had Dr Payne employed negative pressure drains in the primary repair of the incisional hernia Mrs Tinnocks outcome would have been very different to that which inured. I am satisfied that the massive mesh infection and its consequences would have been avoided.
Dr Currer said that use of drains would have reduced a seroma and “might have led to a better control of this infection earlier, it might have led to a lesser infection because the seroma can form a culture medium where bacteria can enhance bacterial growth” (349.34-36 T). He was of the view that the omission to employ drains was probably “one of a number of conditions which were necessary to be present to produce the final outcome that ensued in this case” (349.45-350.3 T). Professor Berney thought that failing to use drains at the original operation and failing to treat the infection more aggressively at an earlier stage possibly contributed in a material way “to the bad outcome in July” (350.50-351.7 T). Professor Morris was of the view that the absence of drains and the failure to adequately treat Mrs Tinnock when she presented with the infection materially contributed to the outcome “simply because the infection of the mesh that occurred was something that was influenced by those … lack of treatments” (351.12-352.4 T).
Dr Miller agreed with Professor Morris with emphasis on the drain. His evidence (352.8-40 T) was:
“My feeling is by not draining this enormous dead space they missed the boat in that if he could have controlled the drainage that would be coming out of that wound post-operatively that it may well have settled over the usual period and therefore the drains would have been removed and there may have been a small residual seroma that could have just been treated conservatively. I think once the boat was missed – there was a window of opportunity to salvage the mesh. And, as Professor Morris sort of has alluded to, the antibiotic period and the rest of it wasn’t followed. So I think not putting the drain in, seroma developed, it was all catch up after that.
…
I think if you had a drain in and you were draining away that collection that became infected that you might get a wound infection or some superficial infection that could be treated with antibiotics because a wound infection is available to the circulation to deliver antibiotics to; whereas a seroma is a large collection and there is no blood supply, so antibiotics can’t get into the centre of it. So if she had developed the infection at the time of the operation – and I am of the view that it occurred when the seroma burst, more likely anyway, because she was sent home without any signs of infection, and, reading the notes it seemed they did have good sterile practice in the operating room.
His Honour: So you say if the seroma had been drained more quickly you think an infection might have been avoided; or if there was an incipient one there, it would have been more easily controlled?
Witness Miller: That’s it.”
Dr Rea accepted that the failure to drain at the incisional hernia repair was a necessary condition of Mrs Tinnock’s condition as it was when she presented at Calvary Hospital, Canberra in July 2010 (349.11-16 T).
I have accepted this evidence in reaching my conclusion about causation expressed above.
The same body of evidence proves that the more aggressive approach of removing the mesh and instituting a more prolonged course of intravenous antibiotics should have been taken when Mrs Tinnock was re-admitted on 3 July 2010. By then aggressive treatment was required but nearly two weeks were lost. Dr Korman also suggested removal of the mesh was necessary at that time (400.22-50T).
DAMAGES
As I have said, by reference to the judgment of Hayne and Bell JJ in Tabet v Gett, in a medical negligence case the relevant injury or harm suffered by the plaintiff will be identified by the comparison between the relevant state of affairs as they existed after the negligent act or omission and the state of affairs that would have existed had the negligent act or omission not occurred.
Had the negligence by omitting to use surgical drains not occurred, the incisional hernia repair undergone by Mrs Tinnock would have been successful and curative of the condition treated, namely the hernia and the disabilities it caused. After a period of convalescence she would have gone on to lead a normal unrestricted life. She would not have required the multiplicity of operations that followed in the event. The state of affairs after the negligence and caused by it is quite different. She underwent an additional five surgical procedures: 15 June 2010; 27 June 2010; 17 July 2010 for wound debridement wash out and removal of the mesh; 14 August 2010 for wound debridement and change of VAC dressing; and 20 July 2011 for revision of the surgical scar by a plastic surgeon. Additionally she was treated for many months, probably until about October 2010, with a cumbersome VAC dressing. She underwent active review and treatment by various medical professionals until about the end of September 2011.
I acknowledge if I am wrong about the use of drains but right about failing to diagnose and aggressively treat the mesh infection the “detrimental difference” caused by the negligence may be somewhat less. For instance, the need to undergo the second and third procedures would not sound in damages. However on the findings I have made as to loss this would result only in a de minimis reduction in quantum.
Mrs Tinnock also claims ongoing pain, discomfort and limitations referrable to her abdominal scar tissue, mechanical back pain, and ongoing consequential psychological injury. She claims to be restricted in the activities of daily life in relation to the performance of domestic chores, impairment of her ability to care for her three children, and a diminution of her earning capacity.
The defendant accepts all the difficulties experienced until the end of 2011. I think it implicit in its position that it accepts a degree of embarrassment about the scarring and some discomfort in that regard. It disputes that the ongoing back problems are related to its negligence and argues that the psychological difficulties are due to other life stressors. The defendant disputes any allowances for economic loss, domestic assistance and child care beyond the end of 2011.
Mrs Tinnock’s background
Mrs Tinnock was born on 31 March 1971 in Perth, Western Australia, as the youngest of five children. She was accordingly 39 at the date of the surgery and is now 46 years of age. She married Paul Tinnock on 8 September 2001 and they had three children together, in June 2006, July 2008 and October 2009.
It is worth recording now that Mrs Tinnock’s evidence was that she and her husband permanently separated in October 2010 due to the stress and strains arising out of her condition due to the negligence of the defendant in 2010. I do not accept this evidence. I accept the argument of the defendant that there were real difficulties in the marriage at least by 6 January 2010 when she consulted her general practitioner Dr Shams, complaining of depression because of her husband’s drinking. She was prescribed medication. She also described herself as separated on the occasion of each admission to Wagga Wagga Base Hospital although she and her husband were apparently sharing the same home. On admission to Calvary Hospital, Canberra on 16 July 2010, she described her domestic situation as living with her children and her ex-husband (Ex AV2 p 252). Indeed the social worker and medical staff at Calvary Hospital assisted in finding community housing for her in Queanbeyan after her first discharge from Calvary Hospital. A letter under the hand of Dr Tom Ward (Ex AV2 p 240) stated:
“Kylie recently had a serious complication after abdominal surgery. To avoid ongoing hospitalisation, she needs to be managed in the community with regular visits from community nurses. At present we understand she doesn’t have accommodation after recently separating from her partner due to concerns about her personal safety and that of her children. With three dependent children under the age of 5 this places her in a difficult situation.
However it is apparent from the evidence that she enjoyed close and substantial support from her parents.
After leaving Woden Valley High School she found work as a sales assistant and made good progress. She later worked as a Commonwealth car driver. She completed a TAFE course in marketing on a part-time basis and obtained courier work with a government department. She later worked in the same department in records management. After her marriage she and her husband relocated to Brisbane. There she continued work in records management on a fulltime basis. After falling pregnant she and her husband returned to the Canberra region where she worked, performing bookwork in her father’s business. The whole family relocated to Wagga Wagga in 2007.
She was out of the workforce while bearing her children and I find because of her incisional hernia would have been unfit for work in any event until it was repaired and she recuperated from surgery, say a period of three months until September 2011.
The plaintiff’s damages are to be assessed in accordance with the provisions of Part 2 of the Act. The main issues in relation to damages for economic loss relate to whether her back pain and psychological condition were caused by the negligence of the defendant.
Damages for non-economic loss
I regarded the plaintiff as a basically honest witness who was doing her best to give an accurate account approximately six years after the relevant events. Because of the effluxion of time, not because of dishonesty, her recollection of events, as will be obvious from what I have already said, was not always accurate. I must say I formed the impression she was a concrete thinker and a rather black and white type of person who tended to be more definite in her answers than perhaps the accuracy of her recall justified. Even so, I thought her account of her symptoms was generally reliable.
She complained of ongoing pain in her abdomen when she moved quickly or attempted to lift heavy objects; very heavy objects caused intense pain. This lead to some limitation in her domestic chores including elevating her hands and arms to hang out the washing or to wash her hair. She experienced some pain in her abdomen every day, sometimes all day. There is extensive scarring in her abdomen which is often itchy. She said she is “repulsed” by the appearance of her scars on her abdomen (Ex B1 [72]). She found the appearance of her scars distressing.
As I have said, she had a sudden onset of back pain during her second admission to Wagga Wagga Base Hospital on 14 June 2010. She did not complain of that matter in her evidentiary statements but mentioned it to the doctors who examined her for the purpose of the case and occasionally has sought treatment for it. There is no issue that she suffers from the condition. The issue relates to its relationship to the defendant’s negligence, as I have already said.
She has complained of back pain in addition to her abdominal pain when consulting her general practitioner. The plaintiff’s counsel pointed to complaints made on 16 March 2011, (Ex AV2 p 361), 30 January 2012 (Ex AV2 p 363), 7 January 2014 and 13 March 2014, 22 May 2014 and 13 June 2014 (Ex AV2 pp 360-364). It is also apparent that the general practitioners involved prescribed strong medication for both her abdominal pain and back pain including, initially, oxycontin and latterly, panadeine forte.
Dr Miller and Dr Dalton who gave evidence about Mrs Tinnock’s general medical condition agreed that she suffered from mechanical back pain probably associated with degenerative changes. In their joint report (Ex F) they agreed that she required ongoing pain management of all of her symptoms including back pain. Both agreed that some of the pain is related to multiple surgeries and complications arising therefrom. Dr Dalton’s view is that the back pain was not specifically related to complications arising from surgery but rather was related to the underlying degenerative changes. He was prepared to accept, however, that the process of deconditioning necessitated by the long series of operations and convalescence from them probably aggravated the pain. Dr Miller was of the view that the course of treatment including the heavy VAC dressing probably had a more active role in aggravating the pain.
I find it unnecessary to go into the detailed evidence they gave before me. It should be said that Dr Dalton was of the view that with appropriate rehabilitation and reconditioning Mrs Tinnock could overcome the back pain.
Given the onset of back pain in June 2010, and having regard to the series of operations and other treatment, I am attracted by Dr Miller’s view. I find that the back pain is a symptomatic aggravation of pre-existing degenerative changes related to the course of treatment necessitated by the defendant’s negligence. The pain may lessen in the future but given it has continued for over six years it is likely to continue indefinitely.
Turning to the psychological consequences, I accept the defendant’s argument that the objective evidence shows that Mrs Tinnock suffered from some depressive symptoms in the six months prior to 7 June 2010. I have made mention of the consultation with Dr Sham on 6 January 2010.
As I understand it, the difference between the psychiatrists, Dr Ackerman and Dr Robertson, is one of emphasis. Dr Ackerman preferred the diagnosis of a major depression and Dr Robertson an adjustment disorder. Dr Robertson initially formed the view that the condition was related to the course of treatment necessitated by the defendant’s negligence and the chronic pain it resulted in but later formed the view that it was due to the sum total of all life stressors to which Mrs Tinnock had been subjected. This, of course, included the course of treatment between 2010 and 2011.
The experts who had previously conferred, undertook a second conference by telephone on 16 March 2016 pursuant to orders made by me to review the cause of Mrs Tinnock’s psychiatric condition. In that conclave they were able to agree that the best description of her condition was “a persistent depressive disorder” (Ex R). Both experts were also able to agree that Mrs Tinnock’s depression “is more attributable to her current circumstances than a direct consequence of the medical negligence”.
I prefer the view of Dr Ackerman that at least much of Mrs Tinnock’s circumstances, especially her experience of pain and other subjective symptoms and disabilities, are referrable to the medical negligence. I accept, as I have said, that the breakdown of her marriage and the adverse impacts of that circumstance are not. If one takes a global view of the position, it is impossible to separate the traumatic circumstances of 2010 and 2011 from the life stressors that together are the cause of her condition. The element of chronic pain should not be sidelined.
I am of the view that her persistent depression is materially contributed to by the negligence of the defendant in the sense that that negligence is a necessary condition of her present psychiatric disorder. It’s notable that Dr Robertson and Dr Ackerman agree that her psychiatric condition is distressing and disabling.
Dr Rea in his report of 11 December 2012 (Ex H) described Mrs Tinnock as having “an evident 25cm long scar situated in the suprapubic region of her abdomen”. There was no umbilicus evident. The centre of the scar was adherent to underlying muscle fascia. He found diminished skin sensation and numbness along the entire length of the scar. He assessed the scarring as constituting severe bodily disfigurement equivalent to 10 per cent of a worst case.
Drawing all these matters together I assess the plaintiff’s non-economic loss as being equivalent to 38 per cent of a most extreme case. As at 1 October 2016, the maximum amount is $605,000.00. At this level there is no applicable ‘deductible’. I will award damages for non-economic loss in the sum of $230,000.00.
Past out-of-pocket expenses
All of the hospital treatment received by Mrs Tinnock was rendered as a public patient and was accordingly free of charge to her. The plaintiff’s schedule of damages refers to a Medicare notice of charge as at 18 May 2015 which was approximately $3,400.00. Additional matters were claimed for medication and supplementation of about $500.00. It seems to me that Mrs Tinnock has not had very active medical treatment in recent years other than the treatment provided by her general practitioner whom she sees frequently for medication. Doing the best I can, I think an allowance should be made on a global basis of, say, $10,000.00.
Future out-of-pocket expenses
A wide range of claims is made for future out-of-pocket expenses relating not only to medical treatment but also to rehabilitation and a number of curative apparati based upon the opinion of the occupational therapist on behalf of the plaintiff, Ms Ravagnani (Ex P). I am not satisfied that all of those aids are called for, nor is every course of treatment recommended likely, in my view, to be undertaken by the plaintiff. She has gone on for several years without the benefit of them and it seems to me unlikely that she will undertake them now. However, some allowance should be made for ongoing general practitioner attendances, medication, psychiatric consultations (which sound very necessary), and rehabilitation including reconditioning. In this regard, I bear in mind that Dr Dalton, a rehabilitation physician, regards Mrs Tinnock, from a physical point of view, as being fit for light semi-sedentary work but in need of re-conditioning. I am of the view that the matter cannot be approached sensibly other than on the basis of a global assessment. I will allow a figure of $30,000.00.
Past economic loss
Mrs Tinnock’s previous employment history is already set out in summary form above. I formed the view that she was a willing and capable worker and from her unchallenged history she seemed to have the ability to progress or be promoted in work she was performing. However, she was probably restricted to the unskilled or semi-skilled areas of employment that she had previously performed including record management and bookkeeping work. Given her social circumstances, I formed the view that she probably would have sought to return to the workforce fulltime after recuperating from a successful incisional hernia repair in or about September 2010. She was totally unfit for work in my view until the end of 2011 because of the treatment necessitated for the avoidable complications of the surgery.
During 2012 she undertook study and acquired the necessary work placements to qualify for a Certificate IV in Community Services work obtained through Goulburn TAFE. The work placements were unpaid. Given that this course of study and experience was by way of mitigation, I think it reasonable as between the plaintiff and defendant for the purpose of assessing damages to continue the period of total incapacity up until approximately the end of 2012.
Her unchallenged evidence is that when last in fulltime employment outside her father’s business around the turn of the century she was earning $700.00 per week net. Making a broad allowance for changes in the value of money until 2010, I think it appropriate to regard her uninjured earning capacity as capable of producing about $1,000.00 per week net on the open labour market but for her injuries. Allowing about two years at that rate until the end of 2012 I will make an allowance for that period of $100,000.00.
The defendant understandably made much of the consideration that the plaintiff was able to work for about 12 months for the St Vincent de Paul Society as a community worker on a casual basis at its Kennedy House institution. Mrs Tinnock had performed a work placement at that organisation during her course and so was familiar with the work. Her application was successful and she was appointed to a position at Hackett in the ACT. It was necessary for her to commute from Goulburn to that position for her shifts. She performed the work for about 12 months and according to her letter of resignation (Ex 8) resigned for “family reasons”. Mrs Tinnock said that she resigned because she was unable to keep up with the work due to her disabilities.
When cross-examined about the family reasons, Mrs Tinnock said “my hernia and my back [are] my family reasons” (176.1 T). The letter also said “my kids are just not dealing with me working” and she accepted that was correct. She accepted that looking after her children was part of the reason why she ceased work. She did not accept that her disability was not the reason for stopping work (176.24-28 T).
On re-examination (182.4-41 T) Mrs Tinnock explained that she wrote the resignation letter after one of her children “bolted”. This was while she was working the night shift and it was in response to that circumstance that she resigned.
I am satisfied that Mrs Tinnock’s chronic pain and her depression impair her capacity to work. Notwithstanding these things I accept, as assessed by Dr Dalton, that she is capable of performing light semi-sedentary work at least on a part-time basis.
Her work at St Vincent de Paul was not fulltime although there were weeks where she worked about 30 hours per week. This was not a constant thing. Her pay details are set out in Ex 6. There were about four weeks where her take home pay was in the vicinity of $800 (she was paid fortnightly). The period covered by Ex 6 shows that Mrs Tinnock earned a total of $14,088.00. This is 18 pay periods during which her average earnings were $782 per fortnight or $391 per week. Obviously that figure may not represent her residual earning capacity given in certain pay periods she clearly was able to earn more.
For the 2013 year during which she worked for St Vincent de Paul I would allow her $600.00 per week for economic loss or $31,200.00. It is not suggested she did not take such work as was offered before she resigned.
I would assess her residual capacity as approximately $500.00 per week net. Despite her family commitments, including the consideration that her second child is on the autistic spectrum, with family help I am of the view that her circumstances would not preclude her from going to work fulltime were she otherwise uninjured. I consider that she continues to have the same impairment of her earning capacity and I would allow past economic loss from 1 January 2014 in the sum of $500.00 per week. The period to the date of judgment is 186 weeks or $93,000.00.
The total allowance for past economic loss is $224,200.00
Employers’ superannuation contribution on past economic loss
Applying the usual rule of thumb of 11 per cent to the amount allowed for past economic loss, I allow $24,662.00.
Future economic loss
There is no reason to suppose that Mrs Tinnock’s symptoms of chronic pain and depression will improve in the short term. However if she undergoes the treatment for which I have provided one would expect improvement in the psychological condition and perhaps through reconditioning a greater capacity to tolerate her ongoing back pain. Given the imponderables attendant upon these matters it seems to me that the proper approach to assessing future economic loss is to make a greater than usual discount for the vicissitudes to take account of the prospect of future improvement and to that end I will adopt a discount for vicissitudes of 25 per cent rather than the conventional 15 per cent.
In accordance with s 13 of the Act, Mrs Tinnock’s most likely future circumstances, but for her injuries, and given the breakdown of her marriage, were to continue in the workforce on a fulltime basis in the type of work she had previously performed. I think she would have been able to manage in this respect with support from her parents while her children were young. Obviously as the children grew into high school age the need for help from her family would have declined.
She will not become eligible for an aged pension until she turns age 67, another 21 years. The 5 per cent multiplier for 21 years is 685.6. Allowing $500.00 per week a gross figure of $342,800 is produced. After deduction of 25 per cent for the vicissitudes I will allow a figure of $257,100 for the future.
Allowance for future employer contributions to superannuation
Given that the rate of the superannuation guarantee charge will increase from 1 July 2020 and thereafter, I will allow a rule of thumb of 14 per cent, a figure of $35,994.
Past domestic assistance
The plaintiff’s need for assistance in the activities of daily living was assessed by Ms Ravagnani for the plaintiff and by Ms Vongdara for the defendant. Both are professional occupational therapists. In accordance with the Court’s directions, the experts conferred and produced a joint report. Regrettably they were not able to agree about much and because of issues about their availability they did not give evidence concurrently. Their joint report is Exhibit 15.
They were able to agree in principle: that Mrs Tinnock required past domestic assistance as a result of her injuries; that she would benefit from some curative apparati, that she required ongoing treatment and management as a result of her injuries; and that she had a need for future care. They were unable to agree about the specifics of the various needs identified.
I also received evidence from Anthony Kilsdonk, Mrs Tinnock’s father and Bridget Kilsdonk, Mrs Tinnock’s mother, about the assistance they provide to her and to the children on a voluntary basis. Mr Kilsdonk is now 73 and Mrs Kilsdonk is 74. I am satisfied that they have rendered a great deal of assistance to Mrs Tinnock personally with her activities of daily living, and provided the care that she was unable to provide to her children because of her disabilities.
The difficulty of course is marrying up their unstinting generosity in providing assistance with objectively assessed needs. I will deal with care of the children separately but it follows from what I have said about economic loss that their assistance with the children would have been required in any event, but for the injury, if Mrs Tinnock worked fulltime, as I have found she probably would have.
Although she underwent five curative procedures, on my findings, Mrs Tinnock was only in hospital for each procedure for a few days. Given the nature of the treatment, the nature of her disabilities and the need to be subject to a VAC dressing for months following July 2010 I am satisfied:
There is a reasonable need for attendant care services to be provided;
That need arose solely because of the injury; and
The services would not have been provided to the plaintiff (at least after September 2010) but for the injury.
Moreover I am satisfied that the services provided cross the intensity and duration thresholds of 6 hours per week and 6 consecutive months respectively required by s 15(3) of the Act. Indeed, on average I am satisfied that for that period from September 2010 when she would otherwise have recuperated from a successful incisional hernia repair, until the end of 2011, those services were provided for not less than 40 hours per week.
As at September 2010, the maximum statutory rate was $996.40 per week and as at 31 December 2011, $1,054.70 per week. I will take the average of $1,025.00 per week and for this 15 month period I will allow 65 weeks at that rate, a figure of $66,625.00.
So far as the period from 1 January 2013 to the present is concerned, I need to take account of the fact that Mrs Tinnock has been much better than she formerly was. She was able to undertake a TAFE course and work placements, and hold down a job for about twelve months. I am of the view that she could continue to work in suitable work on a substantial part-time basis. It must follow from this that despite the help she continues to receive from her parents, she has the capacity to perform a much wider range of domestic chores to look after herself than she did during the acute phase of her injury.
In my view the assessments made by Ms Vongdara in her report of 3 December 2013 (Ex 14), at least so far as they address the position then current, provide a realistic assessment. That assessment of the needs of Mrs Tinnock solely referrable to the services the subject of s 15 of the Act was three hours per week. I have no doubt that much more assistance has been provided by Mrs Tinnock’s parents but in the circumstances I am not satisfied that Mrs Tinnock’s need exceeded the intensity threshold during the period.
The allowance under this head is $66,625.
Future attendant care services
Ms Vongara’s assessment of three hours per week in her view would continue indefinitely into the future. She confirmed that view in the joint report. Ms Ravagnani assessed a range of 4.8 hours per week if rehabilitation had been successful, and 8.3 hours per week if not. However, as I have said, I am of the view that Ms Vongara’s assessment is sensible.
However, it seems unreasonable to expect that Mrs and Mrs Kilsdonk can continue to provide the assistance given their ages. In my view it is both reasonable and probable that Mrs Tinnock, if she has the funds to do so, will arrange for commercial assistance for the heavy household duties, spring cleaning, gardening and heavy lifting that the occupational therapists agree she needs. From the opinions expressed (Ex 15, p 5, [4.5]) I deduce that the experts assess the commercial rate at $45.00 per hour. Bearing in mind the report was written in August 2015 I will increase that to $50.00 per hour. The relevant rate is $150.00 per week on the median life expectancy tables and a woman aged 46 years has a life expectancy of around 42 years. The 5 per cent multiplier is 931.5.
However, doubtless regardless of the negligence of the defendant, as Mrs Tinnock aged she would have had a need for assistance for the very same activities. Accordingly, it is appropriate to discount the allowance to take account of that. I will discount this figure by 33 per cent for the vicissitudes and the allowance is $93,615.75.
Damages under s 15B Civil Liability Act
As at June 2010 Mrs Tinnock had three children under the age of 5 years. Her marriage to her husband had broken down and by reason of the defendant’s negligence her capacity to provide domestic services to her children was impaired. I am satisfied that prior to 7 June 2010 Mrs Tinnock was the primary carer for the children and they were at that time not capable of performing the services she provided by reason of their age, in respect of her first and third child, and by reason of his age and his autism, in the case of her second child. There can be no question that there was a reasonable expectation that but for the injury Mrs Tinnock would have provided the services to her children for at least six hours a week and for a period of at least six consecutive months. Given her virtual total incapacity until about the end of 2011 there was a need for those services to be provided in excess of the intensity and duration thresholds.
In assessing whether an allowance should be made under this head I will bear in mind the provisions of s 15B(10) of the Act and avoid double counting.
I accept that had the incisional hernia repair been a success Mrs Tinnock would have required help with her children until she recovered from the effects of it in or about September 2010. Given the ages of the children I accept that the additional services provided by Mr and Mrs Kilsdonk would have been in the order of 20 hours per week. I appreciate that this means a total of 60 hours of services between them both. However, anyone who has raised young children and provided care for a disabled relative would not think such an assessment unreasonable.
For this period of 65 weeks I will allow half of the maximum statutory rate averaged in the same way as for attendant care services, or $512.50 per week. The amount allowed is $33,312.50.
Insofar as the period from 1 January 2012 is concerned I have borne in mind that I have assessed damages for economic loss on the basis that Mrs Tinnock as a single parent would have worked full time in an occupation comparable to her pre-injury occupation. The evidence also established that Mrs Tinnock had always been close to her parents and it could be expected that they would provide, so far as they were able, assistance to her family. I am not satisfied that she could have worked fulltime unless she had child care assistance either from her parents or from a day care centre.
Moreover, she had recovered by 2012 sufficiently to return to TAFE, perform work placements and in 2013 work in a substantial part-time job including during the night shift. All of this was only achieved with the assistance of her parents. Bearing in mind the need to avoid double counting as required by s 15B of the Act and the consideration that assistance with child care would have been required in any event, I am not satisfied on the balance of probabilities that the intensity threshold has been exceeded after 1 January 2012 solely because of the injuries for which damages are payable. Accordingly, I am not satisfied that I am empowered to make any further allowance for child care services under s 15B of the Act.
Orders
My orders are:
Judgment for the plaintiff in the sum of $1,005,509.00.
The defendant to pay the plaintiff’s costs.
Liberty to apply in respect of arithmetical error in damages calculations and for any special order as to costs.

